Gov. Gretchen Whitmer Releases MI Safe Start Plan to Reengage Michigan’s Economy
May 11, 2020The governor has worked with leaders in health care, business, labor, and education from the Michigan Economic Recovery Council to develop the six-phase plan. The Council, which is also being advised by the Detroit Regional Chamber, Business Leaders for Michigan (BLM), the Grand Rapids Chamber, and the Michigan Chamber of Commerce, is co-chaired by Gerry Anderson, the current chair of Business Leaders for Michigan, and past Chamber Board Chair Nancy Schlichting, the former CEO of Henry Ford Health System (HFHS).
The governor announced that Michigan is currently in phase three, Flattening — the epidemic is no longer increasing and the health system’s capacity is sufficient for current needs.
The phases of the pandemic include:
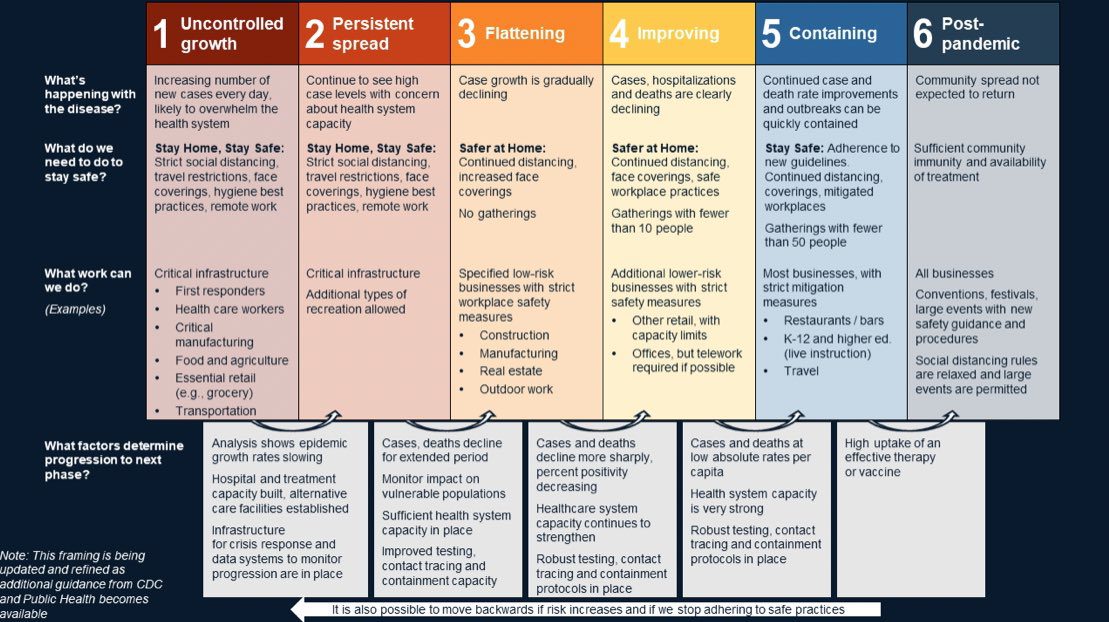
- Uncontrolled Growth: The increasing number of new cases every day, overwhelming our health systems.
- Persistent Spread: We continue to see high case levels with concern about health system capacity.
- Flattening: The epidemic is no longer increasing and the health system’s capacity is sufficient for current needs.
- Improving: Cases, hospitalizations, and deaths are clearly declining.
- Containing: Continued case and death rate improvements, with outbreaks, quickly contained.
- Post-pandemic: Community spread not expected to return.
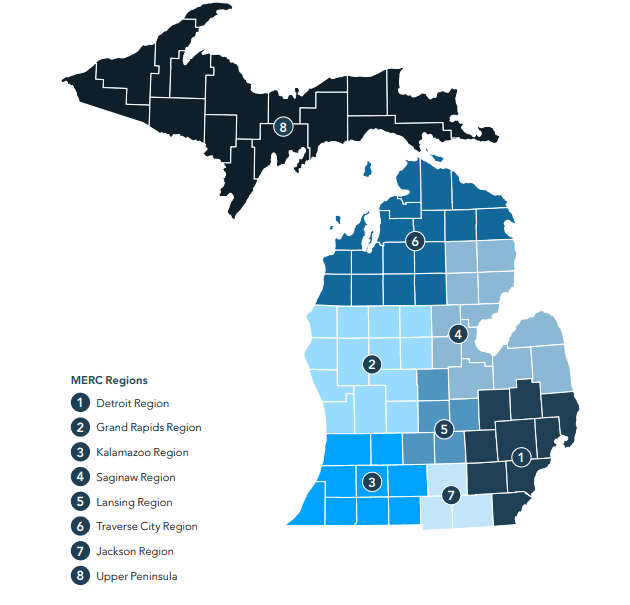
Michigan Economic Recovery Council Reporting Regions
Identified as the MERC regions, the Council broke the state into eight geographical areas that will be used to track the intensity and evolution of COVID-19. When looking at the risk factors of locations, the Council and governor are also considering the health care capacity of the regions as well.
Key Information from the Report
Q: When do we move between phases?
Guided by our public health experts, we are carefully evaluating the best available data to understand the degree of risk and readiness in Michigan. We are complementing that analysis with an understanding of the on-the-ground contextual realities. This comprehensive assessment is a critical input into whether we are prepared to move to the next phase and – just as importantly – whether the disease is surging and we need to adjust our approach.
It is crucial that we monitor the impact of each set of re-engagement activities before moving into the next phase. New transmission can take some time to become visible, and we need to understand any impact of previous re-engagement activities on new disease spread before evaluating a transition to the next stage. As we move into later phases, or if our progress stalls out, it may take longer to move from one phase to another.
Furthermore, it is important to evaluate indicators together: even though some may point to a lower level of risk, others may not. For example, if cases are declining but the health system does not have the capacity to address a sudden uptick in cases, the degree of overall risk may still be high. We will also examine whether different regions within Michigan may be at different phases. That inquiry, too, must be holistic: a region with a low rate of infection may have limited hospital capacity, for example, which puts it at relatively greater risk if an outbreak occurs. Where appropriate, however, regional tailoring makes sense for a state as large and diverse as ours. Examples of the evidence reviewed for each of the three questions is described below:
A. Is the epidemic growing, flattening, or declining?
Evidence analyzed includes:
- The number of new cases per million: low levels of new cases can suggest limited continued transmission; high levels of new cases can suggest continued transmission activity.
- Trends in new daily cases: sustained decreases may suggest that there has not been new takeoff of the disease; increases would provide concern that there has been new takeoff.
- % positive tests: if testing levels are high, a low proportion of positive tests is further evidence of declining spread, and also suggests that we have a good understanding of the state of the epidemic. If there is a high proportion of positive tests, it could suggest further disease spread, or that we have a poor understanding of the true extent of the epidemic.
B. Does our health system have the capacity to address current needs as well as a potential increase, should new cases emerge?
Evidence analyzed includes:
- Hospital capacity: if hospitals are able to surge to accommodate a higher caseload, it suggests that, if a small uptick in new cases occurred during additional re-engagement, our health system would not be overwhelmed. If hospitals are not able to surge in this way, any new case spread could threaten our health system.
- PPE availability: if hospitals have sufficient PPE to manage increased caseloads, it suggests
health system capability to handle a small uptick in new cases.
C. Are our testing and tracing efforts sufficient to monitor the epidemic and
control its spread?
Evidence analyzed includes:
- Testing capacity: if we are able to ensure that the individuals at risk in each re-engagement phase have access to testing when needed, we will be able to give individuals the information they need to stay safe and, at the same time, allow us to closely track the impact of re-engagement activities on our case growth. If we do not have this testing capacity, it will be harder to give our people and our decision-makers the information they need.
- Tracing and containment effectiveness: if we are able to quickly follow up on any newly identified cases and associated contacts, and if those individuals effectively self-isolate, we can more successfully contain any new increase in disease spread. Otherwise, transmission is likely to be higher, increasing our risk.
As new guidance continues to be provided by the CDC and other public health experts, our assessment will adjust to be continually informed by the best available science.
